
Talking to Your Doctor
Talking to a doctor about your pain can be a nerve-wracking experience. Below are some tips to guide a productive conversation about treatment options and promote a positive relationship with your provider.
Prepare Background Information
It’s helpful to prepare some background information for your provider prior to your appointment. The information below can help to establish a treatment baseline.
Describing Your Pain
It’s important for your healthcare provider to have a complete and accurate picture of your pain. Pain is subjective, so tolerance and sensitivity is different for everyone. What you might consider mild pain, someone else could experience as severe pain, and vice versa. It’s crucial, therefore, to consider your pain in terms of multiple criteria:
- Is it tolerable? Can I still do other activities while I’m in pain, even if it’s noticeable or a little distracting?
- What is the sensation of the pain? Does it burn? Is it an ache?
- How would I rate my pain on a normal day on a scale of 1-10? (see sample pain scale below)
- What does a typical day look like for me? Does my pain impact activities? Are there triggers for my pain?
- What’s my treatment history?
Pain Vocabulary
Words matter when describing your pain to your provider. Here are some examples of words you can use to describe your pain:
| Aching | Piercing | Burning | Dull |
| Gnawing | Biting | Hot | Tender |
| Sharp | Shooting | Tingling | Sore |
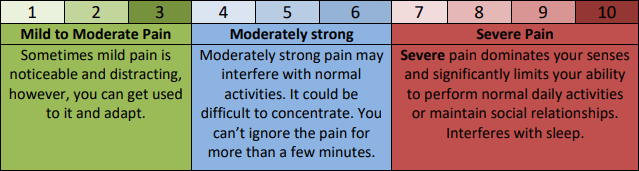
Pain Scale
You may encounter different methods for rating your pain. A common metric is a numerical pain scale, where pain is rated 1-10. Below is a sample pain scale. Don’t be afraid to ask your provider for a more detailed description of the numbers on the scale.
Function vs. Feeling
When describing your pain, it’s helpful to know not only how it feels in your body, but also if and how it limits your ability to do certain activities. It’s important for your provider to get an accurate picture of how your pain impacts your daily life. Some examples of this might be:
- No longer being able to use the stairs because it’s too painful
- Needing help with household chores like laundry and cooking because standing or moving in certain positions hurts too much
- Being unable to work or having to reduce hours or change roles because of pain
Setting Goals
Setting goals is an important first step in the process of chronic pain management. Goal setting serves many purposes:
- Establishes a baseline for pain control strategies by better defining your starting point and the relevant markers of your current lifestyle
- Provides an opportunity to divert your attention from the pain, and shift focus to positive change and achieving milestones
- Helps assess the effectiveness of certain treatment approaches and track your progress
Setting SMART Goals
One standard approach used for setting goals is the SMART method. SMART stands for: Specific, Measurable, Attainable, Relevant, and Time-Bound.
Specific: Goals are clearly defined, detailed, and identify a tangible outcome. You don’t want goals to be too vague.
Measurable: How exactly will you know when you’ve achieved your goal? Success should be clearly defined using relevant metrics.
Attainable: Your goal should be challenging, but still reasonable. When determining if the goal is attainable, start by outlining the steps to achieving it and consider potential barriers.
Relevant: Does this particular goal align with your long-term objectives? Is this the right time to address this goal?
Time-Bound: Set a deadline or target date for achieving your goal. Setting a time-frame for your goal helps to keep you motivated and provide a clear target to work toward.
General Goal Setting Tips
1. Start broadly and then create SMART goals from there. Sometimes the easiest way to create SMART goals is to start with general goals and wants and better defining them from there. For example, you might know that you want to become more physically active. A SMART goal that relates to this broader goal is “Be able to take the dog for a 15 minute walk everyday by the end of July.”
2. Put your goals in writing. Recording your goals and tracking your progress in your journal is a great way to help determine which strategies are having an effect and can provide a safe space to express your feelings about progress or setbacks.
3. Have a mix of short-term and long-term goals. If all of your goals have deadlines too far in the future, it may become discouraging or hard to stay on track if progress feels too far out of reach. Similarly, too many short-term goals can be overwhelming and detrimental to establishing long-term habit changes.
4. Ask for input. Share your goals with your healthcare provider. They’ll be able to offer feedback, insight, and assistance with setting realistic goals.
5. As you work towards your goals, celebrate progress. No progress is too small or trivial to acknowledge. Recognizing your hard work and commitment to achieving your goals is a powerful motivator and mood booster.
Keeping a Journal
Because pain is subjective, it can be challenging to communicate how you’re feeling to your healthcare provider. Prepare for your appointment by tracking your pain for a couple of days prior to your appointment. One method for doing this is by using a pain diary or pain journal. There’s no right or wrong way to journal. You should use a method you are comfortable with and add any additional sections you think could be beneficial. Here are some suggested sections:
Date and Time
Record when you are journaling. We suggest journaling daily to help you more accurately describe how you’re feeling to your doctor, but use your pain diary as you feel comfortable.
Location and Description of Pain
Where in your body are you in experiencing the pain? How would you describe how the pain feels? Different sensations can indicate various root causes of the pain and can be helpful for your healthcare provider in diagnosing the cause of your pain. Record where in your body the pain is located and the best description of the pain.
What Activities are Causing Pain?
Are there activities (e.g. sitting, standing, climbing stairs, household chores) that make the pain worse?
Did You Try Any Treatments?
Are there activities or interventions (e.g. icing/heating, walking, resting, sitting, swimming, yoga, medication) that lessen the pain or improve your ability to cope with the pain? Did you try any treatments that did not impact the pain?
Mood
How are you feeling today? Emotions can often influence how we experience pain just as pain can influence our emotions. Are you stressed, happy, calm, or upset? Record your overall mood for the day in this section.


Bring Someone with You
If you have a partner, roommate, or loved one who has witnessed your pain experience, it’s helpful to bring them with to your appointment (if the clinic allows) so they can provide additional context to your doctor. They can also help record or remember treatment instructions and serve as a support system for you.
If you don’t have someone to accompany you to your appointment, there are resources available like patient advocates whose primary role is to assist individuals in navigating the healthcare system, including dealing with clinicians, understanding your condition and treatment options, and even helping with health insurance issues.
Finding a Patient Advocate
Patient Advocates, or Professional Health Advocates, are represented by three
professional associations: the Alliance for Professional Health Advocates, Greater
National Advocates, and the National Association of Healthcare Advocacy. All three
of these associations have advocate directories that allow you to search for advocates by criteria like location, services and expertise required, etc.
It’s important to note that patient advocates are hired to act in the best interest of the patient, and are not employed by an insurance company or hospital. For that reason, their services are not covered by insurance.
AdvoConnection Directory (Alliance for Professional Health Advocates)
Advocate Search (Greater National Advocates)
Find an Advocate (NAHAC)
Communicate Openly
Your pain is real, regardless of whether or not a root cause can be determined. Preparing background information, creating an external support system and thinking about more detailed ways to describe your pain are strategies to empower you to self-advocate and meaningfully engage with your provider. This can look like building trust, asking questions and being willing to learn, disagreeing, and if necessary, walking away and seeking care from a different provider who might be a better fit.
If you feel your provider is misunderstanding something, say: “Actually, can I clarify this?”
If at the end of the appointment you still feel unheard or that you didn’t receive personalized care, you can say something like: “I’m not feeling good about the direction we’re taking for my care. Can we discuss my concerns?”
It’s crucial to find a provider or team of providers who listen, answer your questions, and validate your concerns, so feel empowered to seek out a second or third opinion if you feel uneasy. You can tell your provider directly by saying: “Thank you for your time today. I think I’d like a second opinion.”
